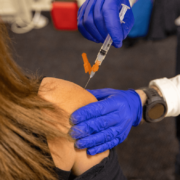
The Consolidated Appropriations Act (CAA) Helps Prevent Surprise Billing
- Find out how the CAA provides relief to individuals by addressing a key health care issue.
- Learn about two common scenarios that create unexpected medical bills for covered employees.
- Find out how the ACA afforded protections against unexpected medical bills and how the CAA addresses additional concerns.
- What can your company do to prepare for compliance procedures that will go into effect in 2022?
By now you’ve likely heard and read much about the Consolidated Appropriations Act (CAA). The CAA provides much-needed relief to individuals and businesses still struggling during the COVID-19 pandemic. A couple of the law’s most talked-about features are stimulus payments to individuals and expansion of the Paycheck Protection Program for businesses.
However, the CAA encompasses many more provisions, affecting everything from disaster losses to retirement plans. It also addresses a key health care issue: surprise billing. If your organization sponsors a group health plan, you may need to take action in the months ahead to comply. Fiducial has highlights on this important part of the CAA and next steps for your compliance.
An ongoing problem
The issue of surprise billing has been slowly but surely gathering momentum for years. The problem: Covered employees suddenly find themselves hit with unexpected medical bills — often several thousand dollars or more.
How does it happen? One common scenario has an employee who needs surgery arranging to have it performed at an in-network hospital by an in-network surgeon. But other members of the surgical team — for example, an anesthesiologist or surgeon’s assistant affiliated with an out-of-network medical practice — also perform services and, boom, the employee is hit with out-of-network charges.
In another typical case, an employee experiences a medical emergency. They are rushed to the nearest hospital — which is, alas, out-of-network. Ambulance and helicopter emergency transit services from non-network providers might also generate surprise bills.

The ACA and the CAA
The Affordable Care Act (ACA) does provide patients some protection in this area. Under the Employee Retirement Income Security Act’s Section 715(a)(1), which was added by the ACA, employers can’t obligate employees to share a greater proportion of the bill for out-of-network emergency medical services than they do for in-network emergency medical services. This rule, however, doesn’t block an out-of-network hospital from billing the employee for the difference between whatever the employer’s plan will pay and the hospital’s total charge.
The CAA goes one step further. It adds provisions that provide that group health plans must implement procedures to prevent surprise medical bills. The effective date of these provisions is any plan year beginning on or after January 1, 2022.
Preventative measures to comply with the CAA
In the coming months, more specifics will likely arise regarding the procedures that employers will need to implement to comply with the CAA. To get a head start, identify the preventative measures against surprise billing that you may already have in place and how they might be enhanced or expanded. Need help managing the costs and financial risks of offering health care benefits? Call Fiducial at 1-866-FIDUCIAL or make an appointment at one of our office locations to discuss your situation.
Ready to book an appointment now? Click here. Know someone who might need our services? We love referrals!
For more small business COVID-19 resources, visit Fiducial’s Coronavirus Update Center to find information on SBA loans, tax updates, the Paycheck Protection Program, paid sick and family leave, and more.